Services
St George’s University Hospitals NHS Foundation Trust is one of London’s leading teaching hospitals with an international reputation for quality of care and cutting-edge treatment. In this area you will find detailed information on all the services we provide. We provide services to both children and adults.
Need to change or cancel your outpatient appointment? You can change or cancel your appointment at St George’s Hospital online via our appointment amendment form.
Filter services
Site
Service
A

Anaesthesia
The Anaesthesia team St George’s Hospital provides expertise in anaesthetic specialties. Our team includes over 100 consultants and 60 trainees from the St George’s School of Anaesthesia.

Audiology and Audiovestibular Medicine
Our Audiology and Audiovestibular Medicine team specialises in diagnosing and managing hearing and balance disorders. We provide specialist care for patients of all ages, offering comprehensive audiovestibular services.

Auditory Implant Service
A cochlear implant is a small, complex electronic device that can help to provide a sense of sound. We offer cochlear implants for both adults and children with profound sensorineural hearing loss.
B

Bereavement Services
If your loved one has died at St George’s, the Bereavement Services team are here to help you. We can guide you through the necessary steps following your bereavement. We also work with clinical teams to ensure that all necessary steps are taken, and paperwork completed.

Breast Service at The Rose Centre
The Breast Service at St George’s is based predominantly at the Rose Centre building which provides a comprehensive service for patients which includes initial consultation and diagnostic services in the same location.
C

Cancer Services
St George’s Hospital serves as a Cancer Centre for South West London, offering high-quality diagnostics, care, and treatments for complex cancer cases. We provide specialised services for regional and supra-regional patients, focusing on complex surgical oncology.

Cardiac Sarcoid Clinic
Our Cardiac Sarcoid Clinic specialises in diagnosing and managing sarcoidosis, particularly when it affects the heart. We provide comprehensive care to manage this rare condition, which involves inflammation and immune cell clusters in various organs.

Cardiac Surgery
St George’s Hospital is a leading centre for cardiac surgery in the southeast of England, performing over 700 operations annually. Our team includes seven consultant cardiac surgeons, supported by a multidisciplinary team of cardiologists, nurses, and other specialists.
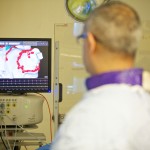
Cardiovascular
Since its first inception in 1954, the St George’s Hospital Cardiology department has been at the forefront of providing pioneering specialist cardiology care to our patients

Care Home Therapy In-Reach
The Care Home Therapy In-Reach team provides therapy support for residents in Wandsworth Older People Care Homes using a holistic, preventative, and collaborative approach.

Carotid atherosclerosis
In conjunction with the regional stroke unit, the St George’s Vascular Institute offers a comprehensive service for patients with carotid atherosclerosis.

Chest medicine
The Respiratory Department at St George’s Hospital offers comprehensive care for respiratory diseases. Our team is dedicated to providing outstanding clinical services for our patients in southwest London and beyond.

Children's services
St George’s University Hospital has a proud history of offering specialist children’s services, providing a mix of care and specialist treatments. We serve children in Wandsworth, Merton, South West London, Surrey, and beyond.

Clinical Pharmacology and Therapeutics
The Clinical Pharmacology and Therapeutics department at St George’s Hospital focuses on the science of drugs and the safe use of medicines. We have one of the largest groups of clinical pharmacologists in the country.

Community services
We provide a full range of community services to patients for people who live and work in Wandsworth, making sure people can manage their health better by accessing the services they need closer to where they live and work, and in their homes.

Covid-19 medicines delivery unit (CMDU)
The Covid-19 medicines delivery unit (CMDU) is based at the Bence Jones Unit, Blackshaw Road, St George’s Hospital. We provide new Covid-19 treatments to people at the highest risk in south west London that have tested positive for Covid-19.
D

Day Surgery Unit
The Day Surgery Unit allows you to be admitted to St George’s Hospital for surgery for a procedure and to be discharged home on the same day. It’s for patients who do not need to stay overnight on a ward and makes the surgery more convenient for them.

Dentistry
Our Dentistry department includes Restorative Dentistry, Orthodontics, and Paediatric Dentistry. We work closely with the Oral and Maxillofacial department to provide comprehensive care.
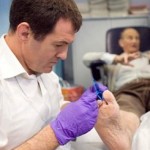
Diabetes and endocrinology
Our Diabetes and Endocrinology departments, located at St George’s Hospital, Queen Mary’s Hospital, and St John’s Therapy Centre, specialise in managing diabetes and hormonal disorders.

Diagnostic services
At St George’s, we provide the following diagnostic services: Blood Testing Services, Cellular Pathology, Haematology, Immunology, Chemical Pathology, Day Case Unit, and Medical Microbiology.
E

Emergency Department (A&E)
Our busy, modern Emergency Department operates 24/7, providing emergency medical care to approximately 150,000 patients annually.

Emergency Department Collaborative Research Group
The Emergency Department (ED) at St George’s leads and participates in a number of research projects through the work of the Collaborative Research Group. The group is part of St George’s Translational and Clinical Research Institute, a joint initiative between the Trust and St George’s, University of London.
G

Gastroenterology
Our Gastroenterology and Hepatology Department teams specialise in diagnosing and treating conditions of the gastrointestinal tract, liver, pancreas, and biliary system.

General Intensive Care
The General Intensive Care Unit (ICU) cares for the most critically ill patients. We diagnose and treat nearly any acute illness using advanced monitoring, organ support therapies, and complex treatments.

General medicine
The General Medicine team provides specialist medical care for a range of conditions, including emergency admissions, gastroenterology, endocrinology, diabetes, respiratory medicine, rheumatology, and cardiology.

Genomics - South West Thames Centre for Genomics
The South West Thames Centre for Genomics at St George’s offers specialised genetic services, including diagnostics and counselling, to patients in South West London, Surrey, and West Sussex. Our UKAS accredited laboratory provides diagnostic analysis and reporting for genetic disorders.

Gynaecology
The Gynaecology service at St George’s and Queen Mary’s Hospitals provides expert care for women’s reproductive health, including diagnosis and treatment of various conditions.
H

Hand Therapy
Our Hand Therapy service helps patients recover from upper limb injuries and conditions, offering a range of therapeutic interventions to restore function.

Hand Unit
The Hand Unit at St George’s Hospital provides comprehensive care for hand and wrist issues, including acute injuries and long term conditions.
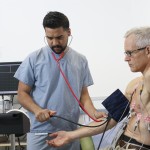
Heart valve centre
The Heart Valve Centre at St George’s Hospital specialises in diagnosing and treating cardiac conditions, including valve diseases, aortic disorders, and arrhythmias.

Hepatology CAS
Our Hepatology Clinical Assessment Service offers specialised care for liver, pancreas, and biliary conditions, streamlining the patient journey from referral to treatment.

Hysteroscopy coordinator
Consultant led. . . .
I

Integrated Sexual Health
The Wandsworth Integrated Sexual Health (WISH) service is now provided by Central London Community Healthcare NHS Trust (CLCH). St George’s continues to provide care for patients with HIV.
For information about sexual health services in south west London, please visit SWISH or Getting It On, or see the CLCH website for details of current services.
L

Learning Disabilities
The Learning Disability team supports patients with learning disabilities and their families, ensuring they receive appropriate care and assistance during their hospital visits.

Liver (Hepatology)
Our Liver service manages a wide range of liver, pancreas, and biliary conditions, including cirrhosis, alcohol-related liver diseases, and liver cancers.

Living with and beyond cancer
The Living with and Beyond Cancer area of the St George’s website is dedicated to providing support to help you to live well after your diagnosis.

Lymphoedema
Our Lymphoedema service provides assessment, diagnosis, and treatment for patients with primary and secondary lymphoedema, offering ongoing support and care.
M

Major Trauma Centre
St George’s Hospital serves as the major trauma center for the South West London and Surrey trauma network. We treat approximately 120 trauma patients monthly, for severe injuries, such as stabbings, gunshot wounds, and serious road traffic accidents.

Make a Tertiary Referral
Pathway for tertiary referral to the pelvic & acetabular team at St George’s hospital. Dial: 0208 672 1255
Bleep: 7064. Monday to Friday (07:30 to 16:00). Your call will be answered by the Pelvic CNS

Maternity
St George’s Maternity Unit offers comprehensive care during pregnancy, birth, and postpartum. We recommend completing an online self-referral form by 7 weeks of pregnancy to schedule your midwife appointment.

Mental Health and Wellbeing
Our Mental Health and Wellbeing service provides support and resources for mental health issues, aiming to improve life expectancy and quality of life for those with serious mental illnesses.

Myoma Service
Consultant led. . . .
N

Neuro-sciences Intensive Care
The Neuro Intensive Care Unit provides a tertiary referral neuroscience acute level of care with physiological monitoring, neurological supportive therapies and complex treatments that necessitate a high staff to patient ratio of a highly skilled, multi-professional team.
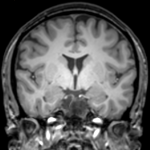
Neurosciences Centre
The Atkinson Morley Regional Neurosciences Centre at St George’s Hospital offers internationally recognised care for neurological conditions, including neurology, neurosurgery, neurorehabilitation, and stroke services. Our comprehensive services cover diagnosis, treatment, and care for disorders of the brain, spinal cord, and nervous system.
O

Occupational health
Our Occupational Health service supports staff health and well-being, offering a range of services to prevent work-related illnesses and manage health issues or disabilities.

Orthotics service
The Orthotic Clinical Service aims to provide a comprehensive inpatient and outpatient orthotic service to aid movement, correct deformity and relieve discomfort. The team specialises in complex rehabilitation problems for patients with musculoskeletal, degenerative and/or neuromuscular problems; many of which utilise our large range of multidisciplinary teams.

Outpatients
St George’s Hospital offers over 1,000 outpatient clinics weekly, providing assessment, diagnosis, and treatment by doctors and specialist nurses.
P

Pharmacy
The Pharmacy Department manages all aspects of medicine use at St George’s Hospital, offering 24/7 services, specialised medicines, and a helpline for medication inquiries.
Plastic and Reconstructive Surgery
Plastic surgery focuses on restoring form and function following injury, illness, or congenital conditions. At St George’s, our specialist team provides a comprehensive range of services, including skin cancer treatment, breast reconstruction, hand and upper limb surgery, and complex reconstructive procedures.
As a major trauma centre for south west London, we manage both planned and emergency cases, working as part of multidisciplinary teams to deliver high-quality, patient-centred care using the latest techniques and innovations.

Prehabilitation before surgery with our Get Set 4 Surgery programme
Our Get Set 4 Surgery programme encourages physical and mental preparation before surgery, aiming to reduce complications and improve recovery outcomes.

Private Patient Service
St George’s welcomes private patients from the UK and abroad. We offer a wide range of advanced treatments and diagnostic procedures and our world-renowned consultants are leaders in their respective fields, treating conditions simple to complex.
R

Rehabilitation services
Our Rehabilitation Service at Douglas Bader Rehabilitation Centre offers specialised care, including prosthetics. The Gait Lab offers detailed walking analysis and functional electrical stimulation (FES) to support neuro-rehabilitation, orthopaedic surgery, and more.

Renal
St George’s Hospital offers comprehensive nephrology services, including kidney transplantation, for patients in South West London, Surrey, and Sussex.

Reproductive Medicine Service
Consultant led. . . .

Resuscitation courses
St George’s Resuscitation Services provide a range of advanced national training courses designed to equip healthcare professionals with the skills needed to manage critically ill patients.
S

Senior health
Our Senior Health service focuses on managing medical and social aspects of illnesses in older adults, providing comprehensive assessments and coordinated care plans.

Social Communication Difficulties Service (including Autism)
Autism is a neurodevelopmental condition that affects how a person communicates, interacts with others, and experiences the world. Every individual is different, and the characteristics of autism can vary widely.
At St George’s, we take a holistic and personalised approach to assessing children and young people, recognising both their needs and their strengths. We work closely with families to provide clear information, guidance, and access to appropriate support services.

South West London Adult Critical Care Network
The SWL Adult Critical Care Network offers specialised intensive care across multiple hospitals, including St George’s, ensuring advanced care for critically ill patients.

Southwest London Post-Covid Specialised Assessment Service
COVID-19 rapid guideline: managing the long-term effects of COVID-19
. . .

Specialist Medicine
Our Specialist Medicine services encompass infectious diseases, dermatology, rheumatology, and hepatitis C treatment, offering both inpatient and outpatient care.

St George's Breast Education Centre Faculty
Our Breast Education Centre offers expertise in breast diagnostics and treatment, with a multidisciplinary team supported by partnerships with Kingston University and St George’s Medical School.

Stop smoking service
We encourage those admitted to the hospital to seek support for quitting or temporary abstinence through nicotine replacement therapy, with the hospital’s stop smoking service offering advice and support during and after your stay.

Surgery
St George’s Hospital offers a wide range of surgical services, including children’s, general, maxillofacial, plastic, pre-operative, and vascular surgery.
T

The Southwest Thames Paediatric Epilepsy Network (SWTPEN)
The South West Thames Paediatric Epilepsy Network (SWTPEN) is a clinical network of healthcare professionals providing care for children and young people with epilepsy across South West London, Surrey and Sussex. The network brings together specialist teams from local hospitals to deliver coordinated, high-quality and accessible care. Its aim is to ensure every child receives consistent, expert support close to home.

Therapies
Therapy Services at St George’s Hospital offer integrated, multi-professional care for inpatients, outpatients, and patients at home. We provide services, such as neurorehabilitation for neurological conditions, and also provide outpatient care and in satellite clinics at GP practices and St John’s Therapy Centre in Battersea

Thoracic surgery
Our Thoracic Surgery service treats chest conditions, including lung cancer, using minimally invasive techniques for both planned and emergency procedures.

Trauma and orthopaedics
The Trauma and Orthopaedics department offers comprehensive care for bone, joint, muscle, ligament, and nerve conditions, including complex surgeries and a dedicated Pelvic Unit.

Tuberous Sclerosis Complex (TSC) Clinic
Our Tuberous Sclerosis Complex (TSC) service provides comprehensive care, addressing non-cancerous growths in various organs. Our team includes specialists from genetics, nephrology, neurology, and more.

Twins Trust Centre for Research and Clinical Excellence
The Twins Trust Centre offers specialised care for multiple pregnancies, including comprehensive antenatal, fetal medicine, and neonatal services.
U

Urology
The Urology Department at St George’s Hospital offers comprehensive services, including advanced robotic surgery using the Da Vinci® Xi robot for cancers and specialised care for benign and malignant urological conditions.
W

Wandsworth Children’s Social Services Occupational Therapy (CSS OT)
Our CSS OT service supports children and young people (0-17 years) with disabilities or long-term conditions, offering assessments, equipment, and adaptations to help manage daily tasks.

Wolfson Outpatient Cognitive Rehabilitation Services (WOCRS)
Wolfson Outpatient Cognitive Rehabilitation Service (WOCRS) is a specialist (Tier 4) service providing assessment and treatment for people with complex cognitive and communication difficulties. Patients are referred for a multidisciplinary assessment, with access to a range of day patient rehabilitation programmes tailored to individual needs.

