Discharge Information
On this page:
Postnatal Information
Congratulations on the birth of your baby. This information (use this link for the PDF version) explains what postnatal care you will receive and provides resources that can show you how to care for yourself and baby at home after birth. If you have any further questions, please speak to your Midwife, GP or Health Visitor.
St George’s Maternity Helpline
Once you are at home, if you have any concerns about you or your baby, please call the Maternity Helpline (open 24/7) to seek advice from a midwife on
020 8725 2777
However, please call 999 for urgent medical attention if:
- Baby stops breathing or goes blue
- Has a fit or convulsion
- Has a rash that does not fade when you press it
- Vomits green fluid
- Is unresponsive / can’t be woken up.
Reasons to seek medical help for your baby
A baby’s illness can become serious if left untreated. The following symptoms can help you decide whether you need to seek medical attention for your baby. Call the Maternity Helpline or your GP if:
- Your baby is less responsive, floppy or difficult to wake
- Pale all over
- Grunts with each breath
- Breathing faster than normal
- Not interested in feeding
- Passes much less urine than normal
- Has a bulging fontanelle (the soft spot at the top of your baby’s head)
- Change in skin colour i.e., yellow (jaundice)
- Has a high or low temperature or is sweating – feels hot or cold to touch
- Has blood in their stools or in the nappy
- If your baby is dehydrated – dry lips and sunken fontanelle.
Reasons to seek medical help for yourself
If you experience any of the following, please come to Delivery Suite triage or call the maternity helpline on 020 8725 2777:
- Severe headaches with or without visual disturbances
- Passing large clots or filling your sanitary pad in an hour with heavy bleeding
- Swelling or pain in your calves
- Offensive smell coming from your perineal stitches or C-section wound.
What care will I receive?
Your community midwife, health visitor and GP will be informed that you have had your baby. You will be seen by a midwife either at home, in a clinic or receive a telephone call the day after you have gone home / had your baby.
The midwife you see will depend on where you live and may not always be from St George’s Hospital. You will be given the relevant contact numbers on your postnatal paperwork. The midwife will then inform you of planned future appointments.
Your baby will be offered Newborn Blood Spot Screening, which must be taken when they are five days old (day of birth is day 0). Please search ‘Screening Tests for You and Your Baby’ or visit this link to access the information online (it is available in other languages too) – Screening Tests For You and Your Baby Information.
You will need to make a GP appointment for yourself at six weeks for a check-up. You will then need to make an additional GP appointment for your baby at eight weeks where your baby will receive another detailed examination. This is also when your baby’s first recommended vaccinations will be due. Whilst we inform your GP that your baby has been born, you will need to register them as a patient at the GP Practice
Registering your baby’s birth

It is a legal requirement to register your baby’s birth within 42 days. Any baby born at St George’s Hospital must be registered at Wandsworth Registry Office. You need to make an appointment online and you will be advised on what you need to take for the registration. Search ‘Wandsworth Registry Office’ online or visit this link to book an appointment to register your baby’s birth.
Caring for your baby at home
New babies have a strong need to be close to their parents, as this helps them to feel secure and loved. This link will take you to the leaflet developed by UNICEF called ‘Building a Happy Baby’ which will provide you with invaluable information and guidance to get started.
How to cope when your baby cries
![]()
Hearing your baby crying can be upsetting, frustrating and at times overwhelming. ICON provides useful information and support to parents on infant crying and how to cope and comfort your baby. Use this link to visit their website.
Where can I get help with feeding my baby?
Please see our infant feeding information on our website by searching ‘St George’s Maternity Feeding Your Baby’ or visiting this link. You will be supported in your feeding choices by our team. The World Health Organisation recommends that your baby requires breastmilk exclusively for the first six months of life and can continue beyond the age of two years old alongside a healthy, balanced diet. We understand that this can be
challenging. It is a process that you and your baby will learn together. If you choose to do combination feeding or exclusive formula feeding, please see the information below.
Community Breastfeeding Support in your Area (2025)
You can contact our infant feeding team on 07766 800 365 or email infantfeeding@stgeorges.nhs.uk if you are experiencing any feeding issues with which your midwife or health visitor has been unable to assist. You can also access a wide variety of multimedia information via the UNICEF website by searching ‘UNICEF Breastfeeding’ online.
Feeding your baby milk from a bottle
If you choose to feed your baby milk from a bottle – whether it be expressed milk or first infant formula, it is very important to prepare the milk in the safest way possible. Please access the St George’s Maternity ‘Feeding Your Baby’ page via this link to see our guidance on cleaning/sterilising and making up feeds.
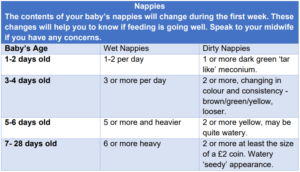
How can I tell if my baby is getting enough milk?
Often the best way to tell is to monitor their wet and dirty nappies. This is a chart that you may find useful. If you are concerned, please ring the Maternity Helpline.
Safe sleeping

The Lullaby Trust provides valuable information about safe sleeping and preventing Sudden Infant Death Syndrome (SIDS). Please access The Lullaby Trust information via this link. The safest way to settle your baby to sleep is as follows:
- In a separate cot or Moses basket in the same room as you for the first six months, even during the day.
- Use a firm, flat, waterproof mattress with NO cushioned areas, pillows, quilts, duvets or bumpers.
- Don’t use any pods, nests or sleep positioners.
- Always place your baby on their back for every sleep, with their feet at the bottom of the cot.
- Do not cover your baby’s head or face while sleeping. Babies should not wear hats when inside.
- Try to maintain the room temperature between 16-20 degrees Celsius, ensuring baby is not too hot or cold.
- Never sleep with your baby on your chest or next to you on a sofa or armchair.
- If you or your partner smoke, drink alcohol or take drugs or are very tired, it is not advisable to share a bed with your baby as this can increase the risk of SIDS. Additionally, bed sharing is not advised if your baby is born prematurely (before 37 weeks) or has a low birth weight (less than 2.5kg / 5lbs8oz).
- If you think your baby is unwell, always seek urgent medical advice.
- Breastfeeding your baby reduces the risk of SIDS.
- Ensuring your baby receives their routine course of vaccinations in their first year of life reduces the risk of SIDS.

Help and emotional support after having a baby
Having a baby can be joyful, exciting, and rewarding. However, it is also common for expectant and new parents to experience anxiety, depression or emotional distress. As many as one in five people experiences emotional difficulties during pregnancy and in the first year after their baby’s birth. This can happen to anyone. Every London borough has an IAPT service which offers free, confidential talking therapy for people who have symptoms of anxiety or depression. IAPT stands for “Improving Access to Psychological Therapy”. IAPT gives priority to expectant and new parents. This link will take you to a leaflet explaining more about the service and the help we can offer you if you need it, alternatively search ‘London IAPT’ online.
Birth reflections
Sometimes following a birth, it is helpful to talk things through – either if things haven’t gone the way you had expected or you just want to reflect on your experience. You can arrange to speak to a Professional Midwifery Advocate (PMA, a senior midwife at St George’s) for a wide range of issues relating to your experience of pregnancy or birth. This is a listening service predominantly but PMAs can answer questions that may arise and follow up on any issues that will improve the quality of our maternity service.
You can contact them by telephone (leaving a message with your name and contact number): 020 8725 2042 or 07826 874 932 or by email: pma@stgeorges.nhs.uk
Postnatal recovery
Your pelvic floor is a group of muscles at the base of the pelvis. They support your pelvis, help to control your bladder and bowel and play a role in sexual function. This link will guide you to the St George’s Pelvic Health Physiotherapy Resources where you can find useful videos and the Postnatal Physiotherapy Advice leaflet.
If you have further concerns or questions, you can contact the Pelvic Health Physiotherapy team on 020 8725 1333. Pregnancy and birth can affect how you move and your bodily functions, such as bladder and bowels. Supporting your body during and after pregnancy is important. This link will take you to the MyHealthLondon video series where more information can be found or search ‘Your Body’s Journey During Pregnancy and After Birth’ online.
Contraception
You can resume sexual intercourse as soon as you feel ready and recovered from the birth of your baby. This should always be your choice. It is also normal to not want to have sex but if this is bothering you, please talk to your GP or visit this link for more information about your contraceptive options from the NHS website. You should start thinking about your contraceptive choices to prevent an unplanned pregnancy. You can become pregnant before your period returns, even if you’re breastfeeding and before you see your GP at your six week check. Your GP will talk to you about your options at this check.
Cervical screening
A cervical screening test or smear test is a method of detecting abnormal (pre-cancerous) cells in the cervix to prevent cervical cancer. The cervix is the entrance to the womb from the vagina. All women aged 25 to 50 are invited for screening every three years and ages 50 to 64 every five years. It is recommended to wait 12 weeks after birth before having your cervical screening if it is due. If you think you are due a smear test, please contact your GP to arrange one. Use this link to go to the NHS web page on cervical screening to find out more information.
Taking medications at home
Following your birth, you or your baby may be prescribed medications to take home. There will be instructions on how to administer these medications on the boxes in which they are given to you. If you are given Fragmin (blood thinning injections) please use this link to find information and guidance about administering your injections.
If you require pain relief during your recovery at home you can take paracetamol and ibuprofen (unless you have been advised otherwise), following the instructions on the packet. You might need to take iron tablets following your birth if you have been diagnosed with anaemia. It is important for it to be most effective that you take it every other day on an empty stomach with a source of Vitamin C like orange juice.
The eRedbook
The eRedbook is the UK’s digital personal child health record. You should receive a paper version of the red book after birth but we advise that you also download the eRedbook from Google Play or the App Store. The eRedbook gives you access to your child’s important health records and helps you track their healthy growth and development. Search ‘eRedbook’ online or visit this link.
St George’s Maternity ‘Going Home Video’
For further important information regarding your discharge, feeding
support and much more watch the St George’s ‘going home’ video
on YouTube via this link.
Contact us
You can call the Maternity Helpline on 020 8725 2777

