Feeding Your Baby
On this page:
You will be supported in your feeding choices by our team. The World Health Organisation recommends that your baby requires breastmilk exclusively for the first 6 months of life and can continue beyond the age of 2 years old alongside a healthy, balanced diet. We understand that this can be challenging. It is a process that you and your baby will learn together. If you choose to do combination feeding, or exclusive formula feeding, please see the information on the ‘Feeding your baby from a bottle’ section.
UNICEF and the WHO recommends exclusively breastfeeding your baby for at least the first six months of their lives followed by the introduction of family foods with the continuation of breastfeeding until two years of age. St George’s Hospital is an accredited UNICEF Baby Friendly maternity service.


What can I do to prepare for breastfeeding?
You can access the following leaflet created by UNICEF: Building a Happy Baby.
You can access feeding information in other languages from UNICEF here: Alternative Language Feeding Information
We have an infant feeding workshop that your midwife can book for you from 34 weeks during your routine appointments, or you can call the infant feeding number: 07766800365
Here are some videos to watch with your support partner about effective feeding, positioning and attachment: Best Beginnings Breastfeeding Videos
Getting breastfeeding off to a good start
Holding your baby in skin to skin contact immediately from birth (where possible) will support your baby’s natural reflexes and instinct to feed from the breast. Skin to skin should be maintained until the baby has finished their first feed, which can typically be between 5-40 minutes.
A useful way to remember the best positioning for a feed is CHINS
- C for close (support your baby close to the breast)
- H for head free (avoid restricting your baby’s head)
- I for in line (align your baby’s ear, shoulder and hip)
- N for nose to nipple
- S for sustainable (are you comfortable?)
Will breastfeeding hurt?
Your nipples can be very sensitive, breastfeeding shouldn’t hurt, although you may feel discomfort at the beginning as you and your baby are getting used to it. It is common to find breastfeeding challenging especially in the early days and feeding journey different. You should always tell your midwife or health visitor if you’re experiencing any issues.
How do I know if my baby is feeding well?
This list is a quick guide to help you assess whether your baby is feeding well:
- Your baby feeds frequently throughout the day (8-12 times in 24 hours
- Your baby is producing a good volume of wet and dirty nappies (see table below)
- Your baby should be gaining weight in line with their birth centile when weighed by a midwife or health visitor
Additional points specific to breastfeeding:
- Your baby is attached deeply at the breast in a position that is comfortable for you both
- Your baby has a strong, rhythmic sucking pattern; and you can see good signs of milk transfer after the colostrum stage (regular swallows and a softening of your breast tissue during the feed)
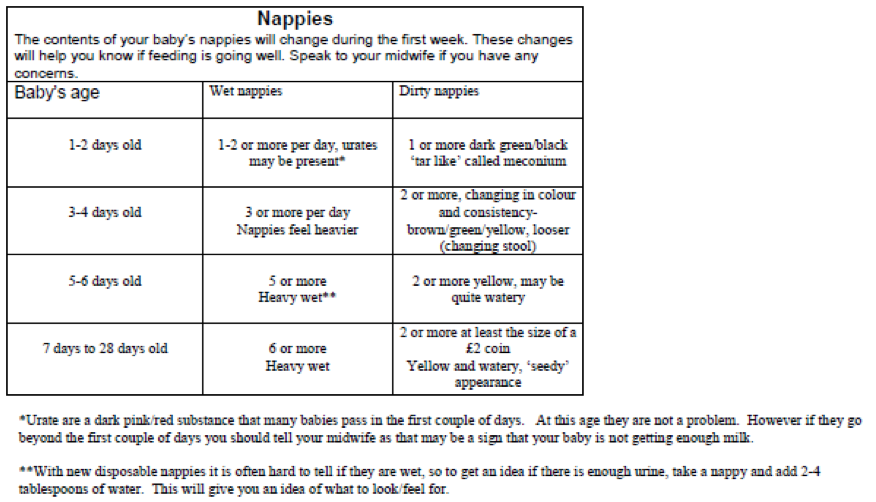
What should my baby’s nappies look like?
This table shows how your babies nappies should look in their first month of life if they are feeding properly.
How will my baby affect my sleep?
Your baby will need to feed, be changed and need comfort regularly through the day and night. If breastfeeding, your lactation hormone levels are higher at night and to maximise your milk supply it is important not to miss these night feeds. For recommendations on how to safely care for and feed your baby at night, see UNICEF ‘Caring for your baby at night’ information here.
What can my partner do to help?
The support of your partner is very important. They can make sure that you are getting enough to eat and drink, can help you by caring for the baby between feeds so you can rest. Your partner can do skin to skin with baby to provide comfort and help them settle to sleep, and they can do care tasks that are necessary like changes, bathing and play.
Feeding your baby milk from a bottle
If you choose to feed your baby milk from a bottle – whether it be expressed milk or first infant formula, it is very important to prepare the milk in the safest way possible.
Will I need to bring in my own formula?
Yes, this is not provided by the hospital. There are no facilities for sterilising bottles on the postnatal ward, so we can supply single use bottles and teats, but you will need to bring in ready-made formula in small cartons or bottles that are typically 70ml.
If your baby requires milk for medical reasons, this will be discussed with you and can be provided. Donor milk or formula milk is available in these medically indicated situations.
Cleaning and sterilising
- Wash your hands and work surfaces
- Clean all feeding equipment in hot soapy water and then rinse under running water before sterilising – remove all traces of milk
- For cold water sterilising units, follow the manufacturers instructions. Change the sterilising solution every 24 hours. Completely immerse the bottles and teats in the solution, ensuring no air is trapped in them. Keep all the equipment under the solution by using the floating cover. It will take a minimum of 30 minutes to sterilise.
- For steam sterilisers, follow the manufacturers instructions. Ensure the openings of the bottles and teats are facing down in the unit. Any equipment not used immediately should be resterilised before use.
Making up formula feeds at home
- Always make up a bottle fresh for each feed, never store milk in the fridge for later as it can grow bacteria that is unsafe for baby.
- You must always use boiled water as tins and packets of milk powder are not sterile, even when sealed. They can contain harmful bacteria which can cause infections that can be life threatening if the feed is prepared incorrectly.
- Use fresh tap water to fill the kettle
- After it is boiled, let it cool for no more than 30 mins. The optimum temperature to prepare the feed is 70 degrees centigrade. Do not use artificially softened water or water that has been repeatedly boiled in the kettle. If you must use bottled water (if you are on holiday), it still needs to be boiled first.
- Stand the sterilised bottle on a clean surface
- Always pour the water first as it is cooling
- Following the formula manufacturer’s instructions, check the bottle is filled to the required level then loosely fill the scoop with milk powder and level it off with the flat side of a clean knife or leveller.
- Never add extra scoops, sugar or cereals to the bottle as this can make your baby ill or choke.
- Carefully attach the teat, retaining ring and cap and shake until all the powder is dissolved.
- Make sure the feed is not too hot – 70 degrees centigrade can still cause scolds. You may need to cool the bottle in cold water before giving to your baby. Always check a small amount on the inside of your wrist to know if it is cool enough for your baby.
What if my baby is in the Neonatal Unit?
If your baby has to have specialist care after birth, you can still breastfeed. Your midwife will help you to hand express colostrum in the early days which can be given to your baby. From 3-5 days after the birth, you can use an electric pump which the midwife or the staff on the Neonatal Unit will show you.
Where can I get help with breastfeeding?
It is perfectly normal to find breastfeeding challenging at first. It is a process that you and your baby learn together. Sometimes issues will arise, but can be resolved with the correct support to enable you to reach your breastfeeding goals. Your community midwife or the Infant Feeding Team can help with breastfeeding support. The Infant Feeding Team are available Monday-Friday 0900-1700 can be contacted on 07766800365 or 020 8725 0199 (answer phone). You or can also get help and further information from a number of other places, including NHS Choices here:
Local breastfeeding support in South West London:
- Please see our Community Breastfeeding Support in your Area Leaflet
Local support organisations:
Telephone support:
- National Breastfeeding Helpline: 0300 1000 0212
- Breastfeeding Network Supporter Line (0930-2130): 0300 1000 0210
Online support:
Facebook: