Tracheostomy tubes
Tracheostomy Tubes
The main components of a tracheostomy tube are universal across the range of designs. The tube shaft is arc shaped and designed as either a single cannula or dual cannula (inner and outer) tracheostomy tube (Fig 3-1). It may have a cuff to provide an airtight seal, to facilitate positive pressure ventilation and reduce the risk of aspiration. For ease of insertion it is supplied with an obturator. The neck flange helps secure the tracheostomy tube to the skin of the neck and stabilise its position.
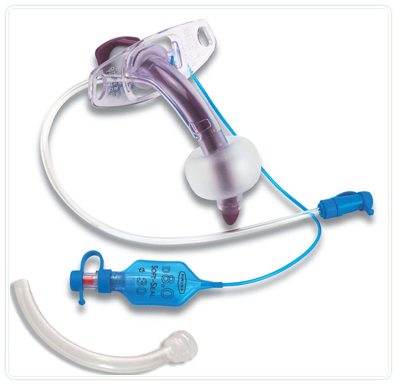
Fig 3-1 Portex® Blue Line Ultra ® tracheostomy tube
Short term tracheostomy tubes have a 15mm connector to allow attachment to airway equipment. Long term tracheostomy tubes may have a low profile flange which is more discreet but cannot be attached to airway equipment. Various tracheostomy accessories exist such as speaking valves, decannulation caps, and HME’s.
Tracheostomy tube dimensions
The length and the diameter of the trachea are roughly proportional to the size of the individual. A tracheostomy tube should be selected according to the outer diameter, the inner diameter and the length of the tube, rather than the manufacturer’s “size”, which is not standardised between models nor manufacturers. i.e. a “size 8” from one manufacturer is likely to have different dimensions to a “size 8” from another (see table 1).
Table 1
Dimensions of some size 8 standard length, cuffed, non-fenestrated tracheostomy tubes. Note the difference in inner diameter (ID), outer diameter (OD) and length.
| ID without inner cannula | ID with inner cannula | Outside diameter | Length | |
|---|---|---|---|---|
| Shiley LPC | n/a | 7.6mm | 12.2mm | 81mm |
| Shiley DCT | n/a | 7.6mm | 12.2mm | 79mm |
| Kapitex Tracheotwist | n/a | 8.0mm | 11.4mm | 76mm |
| Portex Blue Line Ultra | 8.0mm | 6.5mm | 11.9mm | 75.5mm |
The outer diameter of the tracheostomy tube should be about ⅔ to ¾ of the tracheal diameter. As a general rule, most adult females can accommodate a tube with an outer diameter of 10mm, whilst an outer diameter of 11mm is suitable for most adult males.1 A tube should be no wider than necessary in order to minimize trauma to the tracheal wall and long term complications.
The inner diameter of the tracheostomy tube will influence the work of breathing in a spontaneously breathing patient and in turn the course of weaning from the ventilator. Special care is needed when checking the inner diameter of a tracheostomy tube. In the case of a dual cannula tube with the inner cannula in place, the quoted inner diameter on the packaging may or may not reflect this and may be much smaller than anticipated. In accordance with the International Standards Organisation System for size designation, when the 15mm connector is part of the outer cannula, the manufacturer is not obliged to quote the inner diameter of the inner cannula, of which use is optional.
The ideal length of a tracheostomy tube is such that the tube tip lies a few centimeters above the carina. A tube which is too short carries a higher risk of accidental decannulation or partial airway obstruction due to poor positioning. A tube which is too long may impinge on the carina leading to discomfort and coughing.
The tracheostomy tube should be fastened securely to the patient’s neck. Ventilator tubing should be supported to reduce leverage on the tube with risk of tracheal injury and accidental decannulation.
Single and Dual cannula tracheostomy tubes
A non-fenestrated single cannula tube with an air-filled cuff is suitable for most adult patients who require a temporary tracheostomy during critical illness.1
Dual cannula tubes are inherently safer as the inner cannula may be removed quickly in the event of obstruction and are therefore preferred for patients who continue to require a tracheostomy tube after discharge from the Critical Care Unit.1
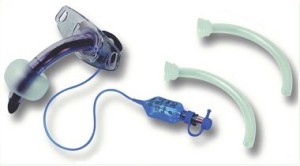
Portex® Blue Line Ultra® dual cannula tracheostomy tube shown with inner cannulae
Staff caring for these patients should be knowledgeable about the design and function of these tubes. The type and size of a tracheostomy tube should be reviewed continuously as a patient’s condition changes. A wide range of specialty tubes are employed to optimise vocalization and comfort.
Fenestrated tracheostomy tubes
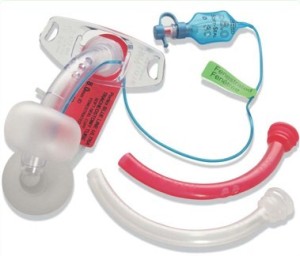
Portex® Blue Line Ultra® fenestrated tracheostomy tube. Multiple fenestrations can be seen. Red colour coded inner cannula has matching multiple fenestrations. Clear white colour inner cannula has no fenestrations.
Fenestrated tubes may be considered for patients undergoing weaning from ventilation, as they facilitate speech and reduce the work of breathing in comparison to non-fenestrated tubes.
Staff should be aware that two types of inner cannulae are supplied with fenestrated tubes; one with a fenestration to promote air flow and speech; and one without a fenestration for suctioning.
Due to the risk of surgical emphysema during positive pressure ventilation even when the non-fenestrated inner cannula is in place, the use of fenestrated tracheostomy tubes is not recommended in newly-formed stomas and should be limited to such time as the wound has healed sufficiently.2
Cuffed tracheostomy tubes
To reduce the risk of tracheal injury, cuff management should include careful inflation technique to the minimal occlusion volume (MOV), followed by monitoring of inflation volume and cuff pressure. The cuff pressure should be maintained between 25-34 cmH2O, but preferably at the bottom end of this range, in order to minimize the risks of both tracheal wall injury and aspiration.3-5
Regular monitoring of cuff pressure is recommended at every shift (8-12 hourly), after any tracheostomy-related intervention, after any change in the cuff volume or upon development of an air leak.3 Common causes of excessive cuff pressure include undersized tracheostomy tube, poor tube positioning, overinflated cuff and reduced lung compliance.
Uncuffed tracheostomy tubes
These tubes are usually used for patients who can protect their own airway, have an adequate cough reflex and most importantly can manage their own secretions. They remove the risk of tracheal damage caused by inflation of the cuff, may aid swallowing and communication with the concomitant use of a speaking valve. However, a speaking valve can only be used in patients who have airflow through their pharynx into their nose and mouth.

Uncuffed Portex® Blue Line Ultra® tracheostomy tube
Uncuffed tracheostomy tubes are frequently used for patients being cared for in the community or a hospital ward. A dual cannula uncuffed tube is preferred for safety and comfort as removal of the inner cannula for cleaning is not traumatic to the patient. Some tubes have low profile openings to make the tube more discreet.
Standard and longer length tracheostomy tubes
Tracheostomy tubes are available in both standard and longer lengths. Standard length tubes are generally designed to accommodate patients with normal airway anatomy. However, the length and angulation of standard design tracheostomy tubes may be too short and unsuitable for some critical care patients, risking complications.6
Longer tracheostomy tubes are available with a fixed or adjustable flange (fixed or adjustable length).
Fixed longer length tubes may be elongated in either the proximal portion (between the stoma and the trachea) or the distal portion of the tube (within the trachea).
Extra proximal length is needed for patients with deep set tracheas i.e. large neck due to obesity, goiter, neck mass. Extra distal length is needed for patients with tracheal problems but normal neck anatomy i.e. tracheomalacia, tracheal stenosis.
A flexible (reinforced) tracheostomy tube with an adjustable flange can be used in any of the above patients, although the locking mechanism of the neck flange may prove cumbersome for the patient, making it less suitable for long term use. In these cases, a dual cannula fixed longer length tube with the appropriate proximal or distal extension for the patient’s anatomy may be more comfortable.
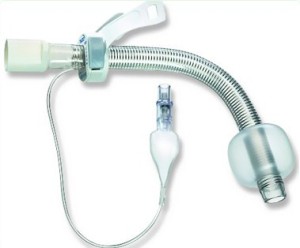
KAPITEX® Traceo vario tracheostomy tube with adjustable flange
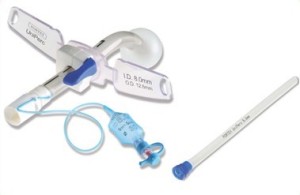
Portex® Uniperc® adjustable flange tracheostomy tube with Soft Seal® Cuff and Inner Cannulae
References
- ICS TICS. Standards for the care of adult patients with a temporary tracheostomy Standards and Guidelines 2008
- Fikkers BG, van Veen JA, Kooloos JG, Pickkers P, van den Hoogen FJ, Hillen B, et al. Emphysema and pneumothorax after percutaneous tracheostomy: case reports and an anatomic study. Chest 2004;125(5):1805-14
- Hess DR. Tracheostomy tubes and related appliances. Respir Care 2005;50(4):497-510
- Crimlisk JT, Horn MH, Wilson DJ, Marino B. Artificial airways: a survey of cuff management practices. Heart Lung 1996;25(3):225-35
- Bernhard WN, Cottrell JE, Sivakumaran C, Patel K, Yost L, Turndorf H. Adjustment of intracuff pressure to prevent aspiration. Anesthesiology 1979;50(4):363-6
- Mallick A, Bodenham A, Elliot S, Oram J. An investigation into the length of standard tracheostomy tubes in critical care patients. Anaesthesia 2008;63(3):302-6

