Bowel symptoms
On this page:
Cancer treatments can cause a range of bowel symptoms including constipation, urgency, and pain. These symptoms might be a result of the cancer itself, treatments such as chemotherapy or radiotherapy, or medications such as hormone suppressors or pain relief.
Below we offer some advice on these symptoms and how to help manage them. Everyone may have different needs relating to their specific cancer or treatment, therefore it is advisable to check advice given with your healthcare team first.
If you have issues with continence of your bowel (e.g. leaking with certain activities or not feeling that you can get clean), you can also have a look at our continence tips page for additional practical advice.
This short film will discuss the below symptoms in more detail and suggest some helpful management strategies!
Constipation
Constipation commonly affects people of all ages. You may have constipation if you are passing stools (poo) less often than usual, or you are finding it more difficult to empty your bowels. Going through cancer treatment is likely to have an impact on your bowels for several reasons, including:
- Medications
- Changes in hormones
- Dehydration
- Reduced exercise or physical movement
- Emotional or psychological impacts e.g. stress or anxiety
How can I help my constipation?
Diet:
- Regular mealtimes
- 5-7 portions of vegetables and fruit each day, unless you have been told to follow a low-fibre diet
- Include wholegrain or wholemeal carbohydrates e.g. brown rice or granary bread
- Introduce fibre gradually
- Some fruit such as apricots, prunes, kiwi’s or figs can naturally help with constipation
- 5-2 litres (5-8 cups) of fluid each day unless your healthcare team tell you differently
Habits:
- A good size breakfast and warm drink can stimulate your gut
- Go when you feel the urge, ignoring this urge can cause the stool to dry out and make it harder to pass
- Try to manage stress and anxiety as best you can
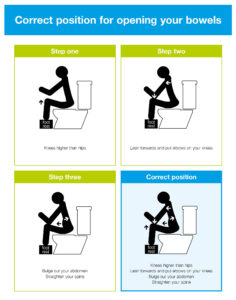
Toilet position:
- Trying to sit in more of a squat position e.g. feet on a stool, can help to relax the pelvic floor muscles to empty your bowels more easily
Diagram reproduced and distributed with the kind permission of the co-authors, including Wendy Ness, Colorectal Nurse Specialist.
Produced as a service to the medical profession by Norgine Ltd. ©2017 Norgine group of companies.
Medications:
- Ask your pharmacist if any of your medications could be contributing to your constipation and discuss with your doctor before stopping any prescribed medication
- Ask your pharmacist about suitable fibre supplements, suppositories or mini-enemas to help you open your bowels for a short-term relief
Diarrhoea
Passing stools (poo) more often than usual or having watery or loose stools. Loose stools increase the risk of leaks as the muscles around our back passage find it much harder to hold onto liquid or gas – see below for further advise on leakage.
How can I help my diarrhoea:
Diet:
- Stay hydrated: aim for at least 2 litres (8+ cups) of fluid each day unless your healthcare team tell you differently
- Eat small and frequent meals if you can tolerate it
- Unless you have been told to follow a low-fibre diet, ensure you have enough fibre in your diet as this helps to bulk up your stool
- Avoid food which irritate the gut such as spicy, greasy, or high-fibre foods
- Homemade rice pudding (using water instead of milk) can be a good meal option if you have loose stools.
Habits:
- Try not to get into the habit of going to the toilet just in case, wait until you feel the urge
- Try to manage stress and anxiety as best you can
Medications:
- Ask your pharmacist if any of your medications could be contributing to your symptoms and discuss with your doctor before stopping any prescribed medication
- Ask your pharmacist about suitable fibre supplements or loperamide to help reduce diarrhoea symptoms
Leakage (incontinence)
Leakage of stool, or wind, from activity or urgency can happen for many reasons. This might include pelvic floor muscle dysfunction, effects of surgery or radiotherapy, previous childbirth, as well as the ageing process. To regain control of your bowels it is important to consider the nutritional, behavioural, and physical components.
Diet:
- Avoid constipation and straining to empty your bowels – this can make things worse in the long-term
- Aim to eat between five and seven portions of vegetables and fruit each day – this will help to ensure your stool remains soft and the skins of fruit and vegetables also provide fibre to bulk your stool
- Ensure your diet also includes some wholegrain or wholemeal carbohydrates (for example brown rice, brown pasta, granary or wholemeal bread etc.). The “husks” cannot be absorbed and therefore add bulk to your stool
- Aim to drink 1.5 litres of fluid each day. This will ensure you are well hydrated and therefore keep your stool soft and help with bowel movement
Habits:
- A good size breakfast and warm drink can stimulate your gut
- Go when you feel the urge, ignoring this urge can cause the stool to dry out and make it harder to pass
- Try to manage stress and anxiety as best you can
Physical:
- Pelvic floor muscle exercises see our pelvic health page for more information on this
- Sphincter exercises can also help you to improve your bowel control. This involves specifically squeezing the muscles around your back passage to build up and strengthen them. See the sphincter exercises page for more information and guidance on how to do these exercises.
- Holding on programme: follow this programme to help to “retrain” your bowels so that you can hold on for longer, reduce leaking, and increase your confidence.
Incomplete emptying
Not feeling empty following bowel movements. This may be due to many reasons such as prolapse (see prolapse section), constipation, altered muscle function, or altered sensation in the rectum.
Your GP, colorectal nurse, or pelvic health physiotherapist can offer further assessment and advice for this.
Difficulty getting clean after bowel movements
If you have had loose stools, haemorrhoids (swollen blood vessels around the anus) or you have weak muscles around the anus then it can sometimes be difficult to get completely clean after a bowel movement.
Try using fragrance free wet wipes instead of toilet roll or splashing cold water over the area. Your GP, colorectal nurse, or pelvic health physiotherapist can also offer further suggestions to help with this.
Bloating and gas
These are common symptoms of cancer treatments, particularly chemotherapy due to the changes in digestion from altered gut bacteria. Strategies to manage these symptoms include eating slowly, avoiding gas-producing foods e.g. beans, pulses, and cabbage, and increasing your physical activity.
You can also speak to your GP or cancer team about potential medications that can help with this.
Pain and cramps
Bowel or tummy pain and cramps are common symptoms of cancer treatments, due to reasons such as inflammation, changes in digestion from altered gut bacteria, constipation and diarrhoea (see above), or occasionally bowel obstruction due to surgical scar tissue (adhesions). It is important that you discuss these symptoms with your GP or cancer team, especially if they are severe or combined with blood in your stool.
Rectal bleeding
This is most common after pelvic radiotherapy due to the irritation to the tissue inside the rectum. It is common but if it becomes persistent or severe then please seek medical attention.
Anal fissures
Tears in the anal skin, which can be painful. These are often caused by radiation, local targeting therapies, or other factors such as chronic constipation. It is important to keep good bowel habits the pelvic health page will provide more information or speak to your GP or cancer team about potential helpful medications.
Stoma care
A stoma is when an opening has been made in the tummy to provide an alternative pathway for waste (poo), and sometimes urine, to leave the body.
These can be temporary, to give the body time to heal, or they can be permanent. A colostomy is an opening in the colon (large intestine) and an ileostomy is an opening in the ileum (small intestines).
Your stoma care nurse will be able to give you more specific advice on managing and caring for your stoma and pelvic health.
Further information

